 To introduce myself first. I am in my early 50s, I have practiced in the same Australian rural center of Emerald nearly 30 years now, first as the local Medical Superintendent than as a General Practitioner for the last 24 years.
To introduce myself first. I am in my early 50s, I have practiced in the same Australian rural center of Emerald nearly 30 years now, first as the local Medical Superintendent than as a General Practitioner for the last 24 years.
I was born in Brisbane but grew up in several country towns Goondiwindi as a preschooler, Roma for my primary years and Longreach for high school. My father was a Policeman and later a Stock Squad Detective chasing Cattle Duffers (His Police car was a 4WD with Quarter horse and Float). My mother was an enrolled nurse at the local Hospital. I studied to Grade 12 as a “Townie” in Longreach and was very lucky to be accepted to Medicine at the University of Queensland.
Studying Medicine as a rural kid back then wasn’t easy, my first plane flight, my first home away from home at College, my first experience of alcohol. It was expensive for my parents so I took a government scholarship.
After a year as an intern in a major City Hospital where I experienced the frank bullying, bastardization and abuse it was a relief to drive into Charleville as a Principal House Officer in my second year; at that time a two doctor hospital to a town of 3000.
Charleville set the scene for me for the rest of my career. I found a home, something that interlopers did not, where I was part of a team of doctors who were both friends and mentors.
Resilience in the face of adversity was something that these people taught me early, as did their partners teach my wife.
Clinical courage, the ability to make decisions in difficult and resource poor settings, was taught implicitly and without rancour.
When we weren’t in Theater we were on the golf course (admittedly under protest, but one did what the local surgeon demanded) or dining together.
Forming lifelong career mentors was important to surviving in isolated practice and I still hold dear the memory of Dr. Louis Ariotti, Professor Jim Baker and the inimitable Dr. Chester Wilson.
We worked long hours but it wasn’t arduous, I did not feel alone nor unsupported.
At one point I did decide that I wanted to do Obstetrics, but the 6 months doing the Diploma of Obstetrics in a City Hospital cured me of ever wanting to return to the viscerally disruptive, soul destroying and impersonal world of hospital and tertiary medicine.
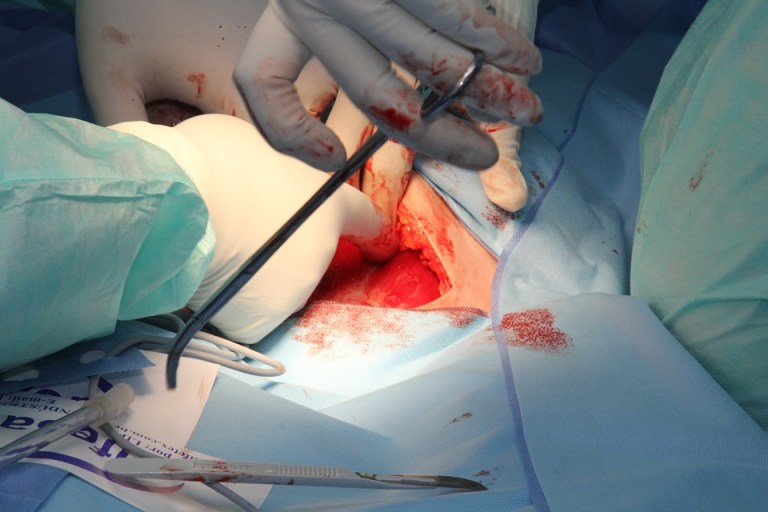
Working at the top end of the scope of clinical practice has been a key feature of my rural life, and one I have expected of the juniors I work with. With 6 weeks of Anesthetics to back me up and no reliable retrieval service I found myself giving a GA for an open Thoractotomy, doing spinal blocks for Cesarean Sections or Total Hip Replacements.
In the first two years of rural practice I had performed over 500 Locals, Sedation’s, Spinals, Epidurals and GAs. I had performed Appendectomy, Cholecystectomy, Gastroscopy. Until recently this vision of a complete rural experience has disappeared at the feet of centralized, “cost effective”, budget centered health systems.
I hope and pray that the rise of Rural Generalist (RG) Medicine will renew what has been lost to rural communities and rural people. The false economy of reducing access to quality primary care in rural areas has produced poorer health outcomes and reduced live expectancy.
What has not been lost on me has been the critical importance of a community and patient centered approach to practice and the critical role of being an advocate for your community.
I often read of anonymity being something precious that clinicians regret surrendering when they life and work in a rural community.
I learnt long ago that having a private life did mean you had to constrain yourself, that you were always on public view as were your family. It has been clear to me that rural practice is more than just a job, you do have an explicit community obligation to serve and your service open to public view as a counter to the elevated position at which the community places you.
![]()
There are new challenges to the public role of a rural doctor as social media, doctors rating sites and other forms of unfiltered public commentary impinge on your own privacy and sense of self.
However a Rural Doctor does has a significant role in the political and cultural life of a rural community. People value your opinion and you can open doors to access to Politicians and Policy advisers and be fearless in your commentary and advocacy.
I have been a small part of the Queensland Rural Doctors movement since its evolution from the Western Queensland Medical Superintendents Association in 1990, and held the second Rural Doctors Association of Queensland conference in my home town.
The rural doctor as Learner and as Teacher has been a key driver for me in becoming a GP supervisor and as a Mentor for quite a few GP and Rural Generalist trainees now. Where I was challenged by the lack of a significant training pathway there now exists real clarity around the discipline of Rural Medicine through the Australian College of Rural and Remote Medicine (ACRRM) and the Royal Australian College of General Practitioners (RACGP) Fellowship of Advanced Rural Practice (FARGP).
In my own town I can relate a recent experience where I was called to see one of my patients in labor. Between the door to ED and the Labor ward though I was invited to review an X-ray by one Doctor and listen to a newborns heart because another Clinician was concerned and wanted a second opinion. I also sought their opinion about the best way to manage an aspect of the labor of my patient, as a shared teacher / learner role exists within the rural clinical culture, and I am never too proud to accept that younger clinicians can bring different and up to date insights to your patient care.
Resilience, working at the top of scope of practice, being a health advocate and a lifelong learner are my most significant memories of rural medicine this last 30 years. However it has not always been a bed of roses.
Isolation, high levels of clinical responsibility, public accountability, accountability to distant administrators and government, and the demands of assessment can create serious mental health problems, stress and burnout.

It is still true that I could say that I was a 30 year “survivor” of rural medicine and that the demands of rural medicine and being a rural doctor are significant. I have cared for a drug dependent colleague, I have dealt with the attempted suicide of some of my colleagues in years past, I have seen peoples careers publicly destroyed by an uncaring and unsympathetic health system.
As we implore young clinicians to live and serve in rural communities so to must we support them, mentor them and understand that their needs are different. I am a dinosaur, a GP whose life is medicine and medicine a calling, a vocation.
I have come to learn about work-life balance, the value of a clinical team and of sharing decisions. Though it might take three clinicians to replace one dinosaur, those three clinicians bring greater clarity, resilience and safety to the care of rural patients. It is critical that health administrators understand that to invest in young clinicians is to guarantee a rural community a more sustainable future.
New technology offers the opportunity to support the clinical courage of rural clinicians, but only if the distant end understands the uniqueness of rural practice. Remote Tele-care cannot replace a rural doctor or nurse, but it can allow that clinician to work to the full extent of their skills. Digital Health is only as useful as the literacy of community and the infrastructure on which it relies; neither is robust in rural practice.
I can only speak of my life as a rural doctor as I haven’t a yardstick to compare it to the life of any other clinician. The above aspects of my lived experience form the key of my understanding of the role that a clinician plays in the community they serve.
Thank you for the shared experiences, wonderful to learn about that side of medicine on that side of the world:).
LikeLiked by 1 person
Thank you Anita, for reading and sharing.
LikeLike
An insightful and generous reflection on rural practice, Ewen. A real pearl…or perhaps dinosaur egg.
LikeLiked by 1 person
Thanks Justin, maybe just a small dinosaur egg 🙂
LikeLike
Thanks Ewen. Really interesting and insightful. I obviously trained around the same time you did (but ended up a townie). I am often glad I didn’t have the same hoops to jump through as young registrars do these days. Pros and cons in the changes as you note.
LikeLiked by 1 person
Do you think the challenges for Townies are any less these days? A good general practice has a generalist multidisciplinary focus regardless of the geography.
LikeLike
Thanks Ewen, I’m an optometrist who has worked beside 3 rural GPS in a small town, with 3 ophthalmologists in a regional centre 37km away. We supported each other and the rural ophthals and stopped many rural people going blind from Glaucoma, ARM and diabetic retinopathy. It was an open process based of patient- centred care and mutual respect. Compared with city practice, it was an exciting challenging and rewarding experience. Rural health disciplines need to support each other and our communities, and fight for decentralisation of money and power in public health.
LikeLike
Yes rural disciplines do need to work across our common focus on rural patients, not our points of difference.
LikeLike